Monday, December 24, 2018
Thursday, December 20, 2018
Who Packs Your Parachute
Living with a progressive neuromuscular condition tends to push a lot of buttons. It is easy to become down, frustrated, angry, feel less than whole, and not see the beauty that surrounds our daily lives.
My brother sent me a story about U.S. Navy pilot Plumb. I found it fascinating and looked online to confirm the story. Kare Anderson wrote in Forbes a good synopsis of Plumb, his story, and his question to all of us.
Charles Plumb was a US Navy jet pilot in Vietnam. After 75 combat missions, his plane was destroyed by a surface-to-air missile. Plumb ejected and parachuted into enemy hands. He was captured and spent 6 years in a communist Vietnamese prison. He survived the ordeal and now lectures on lessons learned from that experience.
The story about Charles Plumb, "Who Packs Your Parachute," is a strong and interesting true story that has been shared with many people over the years during lectures and leadership courses.
One day, when Plumb and his wife were sitting in a restaurant, a man at another table came up and said, “You’re Plumb! You flew jet fighters in Vietnam from the aircraft carrier Kitty Hawk. You were shot down!”
“How in the world did you know that?” asked Plumb.
“I packed your parachute,” the man replied.
Plumb gasped in surprise and gratitude. The man pumped his hand and said, “I guess it worked!” Plumb assured him, “It sure did. If your chute hadn’t worked, I wouldn’t be here today.”
Plumb couldn’t sleep that night, thinking about that man. Plumb says, “I kept wondering what he might have looked like in a Navy uniform: a white hat, a bib in the back and bell-bottom trousers. I wonder how many times I might have seen him and not even said 'Good morning, how are you?’ or anything, because, you see, I was a fighter pilot, and he was just a sailor.”
Plumb thought of the man hours the sailor had spent on a long wooden table in the bowels of the ship, carefully weaving the shrouds and folding the silks of each chute, holding in his hands each time the fate of someone he didn’t know.
Now, Plumb asks his audience, "Who's packing your parachute?" Who has done something that has helped make your day safer – or easier or more pleasant – or who have you witnessed “packing” for someone else?
Each of us are touched by individuals who provide what we need to make it through the day. Some help inadvertently. Praise that person anyway. You are supporting the kind of behavior you respect – making it more likely to happen again.
This is where during Plumb's talks he asks his audience,
We may fail to say "hello," "please," or "thank you," congratulate someone on something wonderful that has happened to them, give a compliment or just do something nice for no reason."
My brother sent me a story about U.S. Navy pilot Plumb. I found it fascinating and looked online to confirm the story. Kare Anderson wrote in Forbes a good synopsis of Plumb, his story, and his question to all of us.
About Charles Plumb
Author Unknown
Charles Plumb was a US Navy jet pilot in Vietnam. After 75 combat missions, his plane was destroyed by a surface-to-air missile. Plumb ejected and parachuted into enemy hands. He was captured and spent 6 years in a communist Vietnamese prison. He survived the ordeal and now lectures on lessons learned from that experience.
The story about Charles Plumb, "Who Packs Your Parachute," is a strong and interesting true story that has been shared with many people over the years during lectures and leadership courses.
Who Packs Your Parachute
"...I was a fighter pilot, and he was just a sailor.”One day, when Plumb and his wife were sitting in a restaurant, a man at another table came up and said, “You’re Plumb! You flew jet fighters in Vietnam from the aircraft carrier Kitty Hawk. You were shot down!”
“How in the world did you know that?” asked Plumb.
“I packed your parachute,” the man replied.
Plumb gasped in surprise and gratitude. The man pumped his hand and said, “I guess it worked!” Plumb assured him, “It sure did. If your chute hadn’t worked, I wouldn’t be here today.”
Plumb couldn’t sleep that night, thinking about that man. Plumb says, “I kept wondering what he might have looked like in a Navy uniform: a white hat, a bib in the back and bell-bottom trousers. I wonder how many times I might have seen him and not even said 'Good morning, how are you?’ or anything, because, you see, I was a fighter pilot, and he was just a sailor.”
Plumb thought of the man hours the sailor had spent on a long wooden table in the bowels of the ship, carefully weaving the shrouds and folding the silks of each chute, holding in his hands each time the fate of someone he didn’t know.
Now, Plumb asks his audience, "Who's packing your parachute?" Who has done something that has helped make your day safer – or easier or more pleasant – or who have you witnessed “packing” for someone else?
Each of us are touched by individuals who provide what we need to make it through the day. Some help inadvertently. Praise that person anyway. You are supporting the kind of behavior you respect – making it more likely to happen again.
This is where during Plumb's talks he asks his audience,
“Who’s packing your parachute?”
Everyone has someone who provides what they need to make it through the day.
Plumb also points out that he needed many kinds of parachutes when his plane was shot down over enemy territory. He needed his physical parachute, his mental parachute, his emotional parachute and his spiritual parachute. He called on all these supports before reaching safety.
Sometimes in the daily challenges that life gives us, we miss what is really important.
We may fail to say "hello," "please," or "thank you," congratulate someone on something wonderful that has happened to them, give a compliment or just do something nice for no reason."
As you go through this week, this holiday season, and this coming year, recognize people who pack your parachute.
The above story is also my way of saying, THANK YOU.
Thank you for reading my blog, for writing me, for providing suggestions and feedback, for everything else you do in "packing my parachute."
Happy Holidays!
Tuesday, December 11, 2018
Symptoms, Diagnosis, and Treatment for SBMA
This is a well written and easy to understand article in Well Written Health.
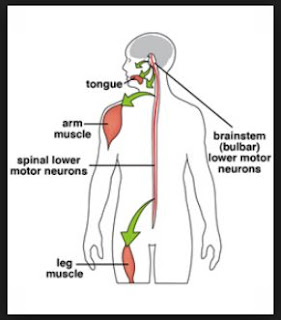
Kennedy disease, also known as spinal bulbar muscular atrophy or SBMA, is an inherited neurological disorder. Kennedy disease affects the specialized nerve cells that control muscle movement (specifically, the lower motor neurons), which are responsible for the movement of many muscles of the arms and legs. It also affects the nerves that control bulbar muscles, which control breathing, swallowing, and talking. Kennedy disease can also lead to androgen (male hormones) insensitivity which causes enlarged breasts in men, decreased fertility, and testicular atrophy.
Kennedy disease is caused by a genetic defect on the X (female) chromosome. Since males have only one X chromosome, they are most severely affected by the disorder. Females, who have two X chromosomes, may carry the defective gene on one X chromosome, but the other normal X chromosome lessens or hides the symptoms of the disorder. Kennedy disease is estimated to occur in 1 in 40,000 individuals worldwide. ...
Often, individuals with Kennedy disease are mistakenly thought to have amyotrophic lateral sclerosis (ALS, or Lou Gehrig's disease). However, ALS, as well as the other similar disorders, does not include endocrine disorders or loss of sensation.
A genetic test can confirm if the Kennedy disease defect is present on the X chromosome. If genetic testing is positive, no other tests need to be done as diagnosis can be made from the genetic test alone. ...
Click on the header link to read the full article.
Symptoms, Diagnosis, and Treatment for SBMA
Kennedy disease, also known as spinal bulbar muscular atrophy or SBMA, is an inherited neurological disorder. Kennedy disease affects the specialized nerve cells that control muscle movement (specifically, the lower motor neurons), which are responsible for the movement of many muscles of the arms and legs. It also affects the nerves that control bulbar muscles, which control breathing, swallowing, and talking. Kennedy disease can also lead to androgen (male hormones) insensitivity which causes enlarged breasts in men, decreased fertility, and testicular atrophy.
Kennedy disease is caused by a genetic defect on the X (female) chromosome. Since males have only one X chromosome, they are most severely affected by the disorder. Females, who have two X chromosomes, may carry the defective gene on one X chromosome, but the other normal X chromosome lessens or hides the symptoms of the disorder. Kennedy disease is estimated to occur in 1 in 40,000 individuals worldwide. ...
Diagnosis of the Condition
There are a number of neuromuscular disorders with symptoms similar to Kennedy disease, so misdiagnosis or under-diagnosis may be common.Often, individuals with Kennedy disease are mistakenly thought to have amyotrophic lateral sclerosis (ALS, or Lou Gehrig's disease). However, ALS, as well as the other similar disorders, does not include endocrine disorders or loss of sensation.
A genetic test can confirm if the Kennedy disease defect is present on the X chromosome. If genetic testing is positive, no other tests need to be done as diagnosis can be made from the genetic test alone. ...
Click on the header link to read the full article.
Monday, December 10, 2018
New Research Could Fine-Tune the Gene Scissors CRISPR
If you are a follower of this blog, you know I am following CRISPR research closely in regards to a potential cure for Kennedy's Disease (SBMA). If this process could reduce the number of CAG Repeats, we might have the cure. One issue that researchers are looking at is how to identify and minimize the potential side effects. Below is a link to the latest article on the fine tuning of the process.
When researchers and doctors use the tool CRISPR to correct genetic errors, it may have side effects on the human genome. Now, researchers from the University of Copenhagen have learned how the molecular machinery behind CRISPR works and thus expect to be able to fine-tune CRISPR and remove the undesired effects.
The introduction of the tool for gene editing, the so-called gene scissors CRISPR, in 2007 was a revolution within medical science and cell biology. But even though the perspectives are great, the launch of CRISPR has been followed by debate, especially focussing on ethical issues and the technology’s degree of accuracy and side effects.
However, in a new study published in the scientific journal Cell researchers from the Novo Nordisk Foundation Center for Protein Research have described how one of the CRISPR technologies, the so-called Cas12a, works – all the way down to the molecular level. This makes it possible to fine-tune the gene-editing process to only achieve the desired effects.
‘If we compare CRISPR to a car engine, what we have done is make a complete 3D map of the engine and thus gained an understanding of how it works. This knowledge will enable us to fine-tune the CRISPR engine and make it work in various ways – as a Formula 1 racer as well as an off-road truck’, says Professor Guillermo Montoya from the Novo Nordisk Foundation Center for Protein Research....
New Research Could Fine-Tune the Gene Scissors CRISPR
GENETIC RESEARCHWhen researchers and doctors use the tool CRISPR to correct genetic errors, it may have side effects on the human genome. Now, researchers from the University of Copenhagen have learned how the molecular machinery behind CRISPR works and thus expect to be able to fine-tune CRISPR and remove the undesired effects.
However, in a new study published in the scientific journal Cell researchers from the Novo Nordisk Foundation Center for Protein Research have described how one of the CRISPR technologies, the so-called Cas12a, works – all the way down to the molecular level. This makes it possible to fine-tune the gene-editing process to only achieve the desired effects.
‘If we compare CRISPR to a car engine, what we have done is make a complete 3D map of the engine and thus gained an understanding of how it works. This knowledge will enable us to fine-tune the CRISPR engine and make it work in various ways – as a Formula 1 racer as well as an off-road truck’, says Professor Guillermo Montoya from the Novo Nordisk Foundation Center for Protein Research....
Molecular Film
The researchers have used a so-called cryo-electron microscope to map the technology. The recently inaugurated cryoEM facility at the University of Copenhagen has established the state-of-the-art technology enabling the researchers to take photographs of the different shapes of the molecule when CRISPR-Cas12a cuts up the DNA strand.
They combined it with a fluorescent microscopy technique called ‘single molecule FRET’ that directly observes the motions of the molecules and the sequence of events for each individual protein.
Among other things, this sequence of events revealed to the researchers that three “pieces” of the CRISPR tools must change form for the DNA to be cut properly.
‘Our new study shows the precise series of events in the genome leading to gene editing. These three “pieces” that change, work like airport security checks. You have to complete all checks and in the right order to proceed’, says Associate Professor Nikos Hatzakis from the Department of Chemistry and the Nano-Science center.
They combined it with a fluorescent microscopy technique called ‘single molecule FRET’ that directly observes the motions of the molecules and the sequence of events for each individual protein.
Among other things, this sequence of events revealed to the researchers that three “pieces” of the CRISPR tools must change form for the DNA to be cut properly.
‘Our new study shows the precise series of events in the genome leading to gene editing. These three “pieces” that change, work like airport security checks. You have to complete all checks and in the right order to proceed’, says Associate Professor Nikos Hatzakis from the Department of Chemistry and the Nano-Science center.
[Click on the link above to read the entire article]
Friday, November 23, 2018
Information Links for Seniors and the Disabled
I received the following email from Richard Wright. I appreciate that he took the time to send these links to me. I hope you find some of these resources informative and useful. Thanks, Richard.
"Since you have so much great info on it [LWKD blog] for individuals who are senior citizens and/or have a disability, I thought you may like to update it with a few additional life- and financial-planning resources I found in my research. They cover a variety of topics, from healthcare and insurance, to home modifications, to canine assistance, and based on the information you’ve already shared on your site, I think they’ll be extremely helpful to your readers.
Here they are:
I hope you can find a way to use these! I’ve also been working on a project where I write articles about how people can create a plan for paying for any future long-term care needs that may arise. If you think an article on that topic would be relevant for your blog, I’d be happy to write a piece for you as well."
Thursday, November 22, 2018
Happy Thanksgiving
In the U.S., it is Thanksgiving. And, it is an opportunity for each of us to count our blessings. It is far too easy to focus on the setbacks and what Kennedy's Disease has done to us. But, when you consider everything else including family, friends, general health, a roof over our heads, food on the table, doctors who care, researchers working on a cure, our freedom, our servicemen and women as well as their families, we have so much to be thankful for.
I could go on, but you get the idea. Thank you for reading my blog posts and commenting. Be safe and stay upright. Bruce
I could go on, but you get the idea. Thank you for reading my blog posts and commenting. Be safe and stay upright. Bruce
Tuesday, November 13, 2018
Researchers Find New Gene That May be Involved in SBMA
The below article was posted by Catarina Silva in SMA News Today. It is a preliminary study that could lead to further research in this particular area. You can read the entire article by clicking on the link below.
"...DHT did not increase SBMA cellular/genetic changes. However, the team found that several genes involved in the regulation of important neurological processes were dysregulated in SBMA spinal motor neurons upon treatment with DHT.
Among these, the FAM135B gene was reduced by more than 10,000-fold in SBMA spinal motor neurons when compared to healthy cells.
Interestingly, this gene was present at low levels in iPSCs derived from either SBMA or healthy individuals. Its differential expression was only observed once these cells became spinal motor neurons, leading researchers to hypothesize that “this gene plays a functional role in supporting sMN [spinal motor neurons] growth and survival.”
To investigate the functional role of this gene in SBMA, the team genetically engineered healthy spinal motor neurons to express lower levels of FAM135B (similar to what was observed in SBMA spinal motor neurons).
The results revealed a decrease in neuronal projections’ length and spinal motor neurons’ survival, suggesting a specific role for this gene in SBMA.
Interestingly, low levels of FAM135B were not observed in amyotrophic lateral sclerosis (ALS) and spinal muscular atrophy (SMA) iPSC-derived spinal motor neurons, indicating that this differential gene expression pattern is unique to SBMA.
“To date there have been no detailed studies that define a role of FAM135B in the nervous system,” researchers said.
“Future work could be focused on detailed investigation of the role of FAM135B in SBMA. With FAM135B proposed to play roles in neuronal survival, growth and maintenance of structural integrity, it could be speculated that an upregulation of which in [spinal motor neurons] could potentially [reverse the disease-related neuronal changes],” they concluded."
Researchers Find New Gene That May be Involved in Spinal and Bulbar Muscular Atrophy Development
"...DHT did not increase SBMA cellular/genetic changes. However, the team found that several genes involved in the regulation of important neurological processes were dysregulated in SBMA spinal motor neurons upon treatment with DHT.
Among these, the FAM135B gene was reduced by more than 10,000-fold in SBMA spinal motor neurons when compared to healthy cells.
Interestingly, this gene was present at low levels in iPSCs derived from either SBMA or healthy individuals. Its differential expression was only observed once these cells became spinal motor neurons, leading researchers to hypothesize that “this gene plays a functional role in supporting sMN [spinal motor neurons] growth and survival.”
To investigate the functional role of this gene in SBMA, the team genetically engineered healthy spinal motor neurons to express lower levels of FAM135B (similar to what was observed in SBMA spinal motor neurons).
The results revealed a decrease in neuronal projections’ length and spinal motor neurons’ survival, suggesting a specific role for this gene in SBMA.
Interestingly, low levels of FAM135B were not observed in amyotrophic lateral sclerosis (ALS) and spinal muscular atrophy (SMA) iPSC-derived spinal motor neurons, indicating that this differential gene expression pattern is unique to SBMA.
“To date there have been no detailed studies that define a role of FAM135B in the nervous system,” researchers said.
“Future work could be focused on detailed investigation of the role of FAM135B in SBMA. With FAM135B proposed to play roles in neuronal survival, growth and maintenance of structural integrity, it could be speculated that an upregulation of which in [spinal motor neurons] could potentially [reverse the disease-related neuronal changes],” they concluded."
Labels:
ALS,
DNT,
FAM135B,
iPSC,
Kennedy's Disease Research,
SBMA,
SMA,
Spinal Bulbar Muscular Atrophy
Wednesday, October 31, 2018
Coping with Change While Changing Beliefs
One of my common themes is “Coping with Change.” Kennedy’s Disease forces you to cope with the unplanned changes in your life. Until you accept the changes, it will be difficult to move forward again. Having a strong belief system is as important as coping.
Spencer Johnson has a way with words. He has written over twenty books and sold tens of millions of copies of Who Moved My Cheese? and The One Minute Manager. Most people have heard of The One Minute Manager, but his second book is not as well known, yet is better for those of us dealing with unexpected change in our lives. You can read the book in an hour or so, but you might find yourself talking about it and reading it again.
“It is an extended allegory based on the experiences of four mice who live in a maze that has cheese located at a particular location. Then one day, the cheese is moved to a new location, and their differing reactions determine their success in the new state of affairs.
In this artful way, Spencer Johnson introduces the reader to his fable on how to cope positively with change. Here is four short quotes from the book.
· “What would you do if you weren't afraid?” ...
· “What you are afraid of is never as bad as what you imagine. ...
· “When you stop being afraid you feel good” ...
· “The quicker you let go of old cheese, the sooner you find new cheese.””
Mr. Johnson passed away in 2017 and left behind the unpublished book, Out of the Maze - This is a story about the power of belief. In this month’s CostCo Connection, Adrian Zackheim writes about “The Power of Story.” It is the long awaited sequel. Adrian Zackheim has taken the drafts and published the book.
“Who Moved My Cheese? offered millions of readers relief for an evergreen problem: unanticipated and unwelcome change. Now its long-awaited sequel digs deeper, to show how readers can adapt their beliefs and achieve better results. Johnson's theme is that all of our accomplishments are due to our beliefs: whether we're confident or insecure, cynical or positive, open-minded or inflexible. But it's difficult to change your beliefs - and with them, your outcomes. Find out how Hem, Haw, and the other characters from Who Moved My Cheese? deal with this challenge.”
Here are six key principles from the book:
· Don’t believe everything you think.
· Old beliefs do not lead you to new beginnings.
· You can change your mind and choose a new belief.
· You are not your belief. You are the person who chooses your beliefs.
· Let go of whatever isn’t working.
· Look outsize the maze. Consider the unlikely, and explore the impossible.
You can find Who Moved My Cheese? at most public libraries or at Amazon. I can’t wait to read the sequel.
Spencer Johnson has a way with words. He has written over twenty books and sold tens of millions of copies of Who Moved My Cheese? and The One Minute Manager. Most people have heard of The One Minute Manager, but his second book is not as well known, yet is better for those of us dealing with unexpected change in our lives. You can read the book in an hour or so, but you might find yourself talking about it and reading it again.
Who Moved My Cheese?
“It is an extended allegory based on the experiences of four mice who live in a maze that has cheese located at a particular location. Then one day, the cheese is moved to a new location, and their differing reactions determine their success in the new state of affairs.
In this artful way, Spencer Johnson introduces the reader to his fable on how to cope positively with change. Here is four short quotes from the book.
· “What would you do if you weren't afraid?” ...
· “What you are afraid of is never as bad as what you imagine. ...
· “When you stop being afraid you feel good” ...
· “The quicker you let go of old cheese, the sooner you find new cheese.””
Mr. Johnson passed away in 2017 and left behind the unpublished book, Out of the Maze - This is a story about the power of belief. In this month’s CostCo Connection, Adrian Zackheim writes about “The Power of Story.” It is the long awaited sequel. Adrian Zackheim has taken the drafts and published the book.
Out of the Maze
“Who Moved My Cheese? offered millions of readers relief for an evergreen problem: unanticipated and unwelcome change. Now its long-awaited sequel digs deeper, to show how readers can adapt their beliefs and achieve better results. Johnson's theme is that all of our accomplishments are due to our beliefs: whether we're confident or insecure, cynical or positive, open-minded or inflexible. But it's difficult to change your beliefs - and with them, your outcomes. Find out how Hem, Haw, and the other characters from Who Moved My Cheese? deal with this challenge.”
Here are six key principles from the book:
· Don’t believe everything you think.
· Old beliefs do not lead you to new beginnings.
· You can change your mind and choose a new belief.
· You are not your belief. You are the person who chooses your beliefs.
· Let go of whatever isn’t working.
· Look outsize the maze. Consider the unlikely, and explore the impossible.
You can find Who Moved My Cheese? at most public libraries or at Amazon. I can’t wait to read the sequel.
Wednesday, October 24, 2018
BVS857 Clinical Trial Yields Mixed Results
Below is another article reporting the results of the BVS857 Trial. Click on the link to read the article at SMA News Today.
Novartis Pharmaceuticals‘ investigational compound BVS857 significantly improved muscle volume in patients with X-linked type spinal muscular atrophy (SMA) over a short period of time, Phase 2 clinical results show. However, the compound failed to improve muscle strength and function.
These findings were reported in the study, “Safety, tolerability, and preliminary efficacy of an IGF-1 mimetic in patients with spinal and bulbar muscular atrophy: a randomised, placebo-controlled trial,” published in The Lancet Neurology.
X-linked type SMA, also known as spinal and bulbar muscular atrophy (SBMD), or Kennedy’s disease, is caused by a faulty androgen receptor (AR) gene and is characterized by degeneration of muscle and lower motor neurons of the brain stem and spinal cord.
Previous studies have shown that patients with this disease have low amounts (less than 170 ng/mL) of insulin-like growth factor-1 (IGF-1) in the blood. Also, cellular and mouse studies have suggested that by increasing the amount of this signaling molecule it may be possible to ease the features of AR gene mutations.
IGF-1 is a growth factor with different roles in many aspects of childhood growth. It also plays an important role in adult metabolism.
Novartis developed the artificial compound BVS857 specifically to mimic the natural activity of the IGF-1 hormone, while holding enhanced efficiency. This molecule is capable of IGF-1 receptor activation, but has a longer half-life — the time it takes for the body to eliminate half of the substance — than IGF-1.
The safety and effectiveness of BVS857 was evaluated in a Phase 2 trial (NCT02024932) in adult patients with genetically confirmed Kennedy’s disease recruited at six clinical sites in Denmark, Germany, Italy, and the United States. Patients were at least 18 years old, were ambulatory, had muscle weakness and IGF-1 blood serum levels below 170 ng/mL.
The study was divided into two parts. The first part included eight patients who received increasing doses of the investigational compound or a placebo. In the second part, 27 patients received weekly intravenous injections of 0.06 mg/kg BVS857 or placebo for up to 12 weeks.
During the study 89% and 94% of the patients in the placebo and BVS857 groups, respectively, experienced at least one adverse side effect, with the proportion of moderate adverse side effects being higher in the BVS857-treated group.
The most common treatment-related side effects were inflammation of the nose and pharynx, and headache. In general the treatment was found to be safe without inducing any serious problems.
Repeated treatment with BVS857 induced a significant increase in IGF-1 levels up to a mean value of 788 ng/mL.
Evaluation by magnetic resonance imaging (MRI) scans revealed that BVS857 could induce a significant, but mild, improvement of thigh muscle volume (TMV) — a marker of muscle wasting — compared to initial values. Also, TMV in BVS857-treated patients remained stable during the trial, while it decreased in the placebo group.
However, new assessment of TMV approximately 21 and 48 days after completion of the treatment showed no significant differences between the two groups.
BVS857 also failed to induce significant improvements on disease symptoms, as determined by the Adult Myopathy Assessment Tool score, and lean body mass when compared to placebo after 12 weeks.
“Overall, no significant differences were found in any of the motor functional measures between the BVS857 and placebo groups,” researchers wrote.
During the trial, about 72% of the patients on the BVS857 treatment group developed antibodies against both the investigational compound and natural IGF-1, which in 46% of the cases had a neutralizing effect. This enhanced immunoreactivity was fully resolved upon treatment discontinuation.
Collectively, these results demonstrated that IGF-1 pathway activation over a short period of time can significantly improve muscle volume in patients with Kennedy’s disease. Still, it failed to improve muscle strength and function.
“The evidence of preliminary efficacy over the short timeframe of 12 weeks in this study is encouraging and not previously described,” researchers wrote. “Activation of the IGF-1 pathway by other means, perhaps in combination with an anti-androgen drug, might be worth pursuing in future clinical trials.”
“We believe this result has implications for other clinical proof-of-concept studies in patients with muscle atrophy or wasting,” researchers concluded.
BVS857 Clinical Trial Yields Mixed Results
BY ALICE MELÃONovartis Pharmaceuticals‘ investigational compound BVS857 significantly improved muscle volume in patients with X-linked type spinal muscular atrophy (SMA) over a short period of time, Phase 2 clinical results show. However, the compound failed to improve muscle strength and function.
These findings were reported in the study, “Safety, tolerability, and preliminary efficacy of an IGF-1 mimetic in patients with spinal and bulbar muscular atrophy: a randomised, placebo-controlled trial,” published in The Lancet Neurology.
X-linked type SMA, also known as spinal and bulbar muscular atrophy (SBMD), or Kennedy’s disease, is caused by a faulty androgen receptor (AR) gene and is characterized by degeneration of muscle and lower motor neurons of the brain stem and spinal cord.
Previous studies have shown that patients with this disease have low amounts (less than 170 ng/mL) of insulin-like growth factor-1 (IGF-1) in the blood. Also, cellular and mouse studies have suggested that by increasing the amount of this signaling molecule it may be possible to ease the features of AR gene mutations.
IGF-1 is a growth factor with different roles in many aspects of childhood growth. It also plays an important role in adult metabolism.
Novartis developed the artificial compound BVS857 specifically to mimic the natural activity of the IGF-1 hormone, while holding enhanced efficiency. This molecule is capable of IGF-1 receptor activation, but has a longer half-life — the time it takes for the body to eliminate half of the substance — than IGF-1.
The safety and effectiveness of BVS857 was evaluated in a Phase 2 trial (NCT02024932) in adult patients with genetically confirmed Kennedy’s disease recruited at six clinical sites in Denmark, Germany, Italy, and the United States. Patients were at least 18 years old, were ambulatory, had muscle weakness and IGF-1 blood serum levels below 170 ng/mL.
The study was divided into two parts. The first part included eight patients who received increasing doses of the investigational compound or a placebo. In the second part, 27 patients received weekly intravenous injections of 0.06 mg/kg BVS857 or placebo for up to 12 weeks.
During the study 89% and 94% of the patients in the placebo and BVS857 groups, respectively, experienced at least one adverse side effect, with the proportion of moderate adverse side effects being higher in the BVS857-treated group.
The most common treatment-related side effects were inflammation of the nose and pharynx, and headache. In general the treatment was found to be safe without inducing any serious problems.
Repeated treatment with BVS857 induced a significant increase in IGF-1 levels up to a mean value of 788 ng/mL.
Evaluation by magnetic resonance imaging (MRI) scans revealed that BVS857 could induce a significant, but mild, improvement of thigh muscle volume (TMV) — a marker of muscle wasting — compared to initial values. Also, TMV in BVS857-treated patients remained stable during the trial, while it decreased in the placebo group.
However, new assessment of TMV approximately 21 and 48 days after completion of the treatment showed no significant differences between the two groups.
BVS857 also failed to induce significant improvements on disease symptoms, as determined by the Adult Myopathy Assessment Tool score, and lean body mass when compared to placebo after 12 weeks.
“Overall, no significant differences were found in any of the motor functional measures between the BVS857 and placebo groups,” researchers wrote.
During the trial, about 72% of the patients on the BVS857 treatment group developed antibodies against both the investigational compound and natural IGF-1, which in 46% of the cases had a neutralizing effect. This enhanced immunoreactivity was fully resolved upon treatment discontinuation.
Collectively, these results demonstrated that IGF-1 pathway activation over a short period of time can significantly improve muscle volume in patients with Kennedy’s disease. Still, it failed to improve muscle strength and function.
“The evidence of preliminary efficacy over the short timeframe of 12 weeks in this study is encouraging and not previously described,” researchers wrote. “Activation of the IGF-1 pathway by other means, perhaps in combination with an anti-androgen drug, might be worth pursuing in future clinical trials.”
“We believe this result has implications for other clinical proof-of-concept studies in patients with muscle atrophy or wasting,” researchers concluded.
Friday, October 19, 2018
Trial Shows Positive Initial Results for IGF-1
This is a follow-up article written by Lucy Piper on the IGF-1 trials that is written more for the layperson. It was published in Medwire News. Click on the link below to read the article at Medwire.
“By targeting the IGF-1 pathway in spinal and bulbar muscular atrophy, we aimed to replenish the reduced IGF-1 concentrations found in this disease, to stimulate downstream Akt activity to reduce the toxicity of the mutant androgen receptors, and to increase anabolic activity to prevent muscle loss”, the researchers explain.
They examined the tolerability and preliminary efficacy of the IGF-1 mimetic BVS857 in 27 patients, of whom 18 who were randomly assigned to receive the drug while nine were assigned to placebo.
The patients, aged at least 18 years, were ambulatory, had symptomatic weakness and had serum IGF-1 levels of 170 ng/mL or below.
The patients given BVS857 0.06 mg/kg intravenously once a week for 12 weeks showed a significant improvement from baseline in thigh muscle volume – a marker of muscle wasting and denervation – on magnetic resonance imaging scans, compared with placebo, with a geometric mean ratio of 1.04 in favour of the treatment.
Specifically, thigh muscle volume remained stable in the patients taking BVS857, whereas it declined in the placebo group over the course of treatment.
Improvements in the Adult Myopathy Assessment Tool score were seen in both groups, at 7.0% in the placebo group and 4.9% in those taking BVS857, but there was no significant difference between the two. There was also no change in lean body mass in either group.
There was a similar positive change in EQ-5D score for the two groups and a significant improvement with BVS857 over placebo in SF-36 Mental Component Score.
The researchers, led by Christopher Grunseich (National Institutes of Health, Bethesda, Maryland, USA), note in The Lancet Neurology that there was no treatment effect on muscle function, which may be “a consequence of the small effect on muscle volume.” And there was no increase in Akt signalling in monocytes or muscle biopsy samples possibly as a consequence of “the short duration of the increase in total IGF-1 equivalency”, they propose.
In a related commentary, Atsushi Hashizume and Masahisa Katsuno, both from Nagoya University Graduate School of Medicine in Japan, say that the discrepancy between a positive drug effect on thigh muscle volume and clinical outcomes “suggests a need for identification of novel biomarkers that reflect both biological and clinical effects of IGF-1 mimetics and related drugs.”
They add that “extension of the half-life of IGF-1 is key to improving the biological effects of this therapy in patients with spinal and bulbar muscular atrophy.”
BVS857 was otherwise generally well tolerated, with no cases of hypoglycaemia, Bell’s palsy or serious adverse events. However, immunogenicity was detected in 72% of patients taking BVS857, which “limits its use as a therapeutic drug”, note Grunseich and team.
They conclude that the findings are “encouraging” and call for further trials with sufficient power and longer duration to better assess the effects of IGF-1 targeting on muscle strength and function.
“Activation of the IGF-1 pathway by other means, perhaps in combination with anti-androgen drug[s], might be worth pursuing in future trials,” they suggest.
By Lucy Piper
medwireNews (www.medwireNews.com) is an independent medical news service provided by Springer Healthcare. © 2018 Springer Healthcare part of the Springer Nature group
Positive initial results for IGF-1 pathway as treatment target in spinal and bulbar muscular atrophy
medwireNews: The insulin-like growth factor-1 (IGF-1) pathway may be a suitable treatment target for patients with spinal and bulbar muscular atrophy, suggest preliminary findings.“By targeting the IGF-1 pathway in spinal and bulbar muscular atrophy, we aimed to replenish the reduced IGF-1 concentrations found in this disease, to stimulate downstream Akt activity to reduce the toxicity of the mutant androgen receptors, and to increase anabolic activity to prevent muscle loss”, the researchers explain.
They examined the tolerability and preliminary efficacy of the IGF-1 mimetic BVS857 in 27 patients, of whom 18 who were randomly assigned to receive the drug while nine were assigned to placebo.
The patients, aged at least 18 years, were ambulatory, had symptomatic weakness and had serum IGF-1 levels of 170 ng/mL or below.
The patients given BVS857 0.06 mg/kg intravenously once a week for 12 weeks showed a significant improvement from baseline in thigh muscle volume – a marker of muscle wasting and denervation – on magnetic resonance imaging scans, compared with placebo, with a geometric mean ratio of 1.04 in favour of the treatment.
Specifically, thigh muscle volume remained stable in the patients taking BVS857, whereas it declined in the placebo group over the course of treatment.
Improvements in the Adult Myopathy Assessment Tool score were seen in both groups, at 7.0% in the placebo group and 4.9% in those taking BVS857, but there was no significant difference between the two. There was also no change in lean body mass in either group.
There was a similar positive change in EQ-5D score for the two groups and a significant improvement with BVS857 over placebo in SF-36 Mental Component Score.
The researchers, led by Christopher Grunseich (National Institutes of Health, Bethesda, Maryland, USA), note in The Lancet Neurology that there was no treatment effect on muscle function, which may be “a consequence of the small effect on muscle volume.” And there was no increase in Akt signalling in monocytes or muscle biopsy samples possibly as a consequence of “the short duration of the increase in total IGF-1 equivalency”, they propose.
In a related commentary, Atsushi Hashizume and Masahisa Katsuno, both from Nagoya University Graduate School of Medicine in Japan, say that the discrepancy between a positive drug effect on thigh muscle volume and clinical outcomes “suggests a need for identification of novel biomarkers that reflect both biological and clinical effects of IGF-1 mimetics and related drugs.”
They add that “extension of the half-life of IGF-1 is key to improving the biological effects of this therapy in patients with spinal and bulbar muscular atrophy.”
BVS857 was otherwise generally well tolerated, with no cases of hypoglycaemia, Bell’s palsy or serious adverse events. However, immunogenicity was detected in 72% of patients taking BVS857, which “limits its use as a therapeutic drug”, note Grunseich and team.
They conclude that the findings are “encouraging” and call for further trials with sufficient power and longer duration to better assess the effects of IGF-1 targeting on muscle strength and function.
“Activation of the IGF-1 pathway by other means, perhaps in combination with anti-androgen drug[s], might be worth pursuing in future trials,” they suggest.
By Lucy Piper
medwireNews (www.medwireNews.com) is an independent medical news service provided by Springer Healthcare. © 2018 Springer Healthcare part of the Springer Nature group
Image: https://www.alpco.com/role-igf-1-growth-hormoneigf-axis
Thursday, October 18, 2018
Update on the Use and Cost of Orphan Drugs
If a treatment or cure for Kennedy's Disease (SBMA) is found, the orphan drug act will be helpful. Below is an update from NORD.
The major findings of the report are as follows:
“2017 was a year of innovation and advancements in rare diseases, with more FDA approvals of treatments for rare diseases than ever before,” said NORD President and CEO Peter L. Saltonstall. “The recent IQVIA Institute study highlights the enduring importance of the Orphan Drug Act in making that progress possible.”
“It is critical to note that orphan drugs remain a sliver of overall drug spending in the U.S.,” Saltonstall said. “NORD remains committed to shining a light on the simple truths that illustrate how the Orphan Drug Act continues to be vital to the future of rare disease drug research and development.”
About 7,000 rare diseases have been identified, affecting approximately 30 million Americans. Many affect only a few hundred or a few thousand individuals. Rare diseases tend to be chronic, serious and life-threatening. More than 80 percent are believed to be genetic.
Information on the report, including a link to the study, is available on the NORD website at www.rarediseases.org/rareinsights.
Updated Study Analyzes Use and Cost of Orphan Drugs
Median annual cost for top 10 rare disease therapies is less than $10,000 per year
Washington, D.C., October 18, 2018— Despite a record-breaking number of new approvals, orphan drugs remain a nominal part of overall drug spending, accounting for only 9.6% of total sales in the U.S. in 2017, according to a new study released today by the IQVIA Institute. The study was commissioned by the National Organization for Rare Disorders (NORD) for the second year in a row to show trends in orphan drug usage and costs.The major findings of the report are as follows:
- The Orphan Drug Act remains successful in encouraging the development and approval of orphan drugs. In 2017, the Food and Drug Administration approved 80 orphan indications and 57 just within the first eight months of 2018 -- shattering previous records.
- The Orphan Drug Act has not been a major driver of drug pricing in the U.S. In 2017, the median price of the top 10 rare disease therapies used by the greatest number of patients was less than $10,000 per year.
- In 2017, orphan drugs remained a small part of the overall medicine budget. Total drug spending in the United States in 2017 was $451 billion, with almost 56% spent on non-orphan traditional drugs, 34.7% spent on non-orphan specialty drugs and 9.6% spent on orphan indications of approved orphan drugs. That is a 1.7 percentage point increase over 2016, which is in line with increased FDA approvals.
“2017 was a year of innovation and advancements in rare diseases, with more FDA approvals of treatments for rare diseases than ever before,” said NORD President and CEO Peter L. Saltonstall. “The recent IQVIA Institute study highlights the enduring importance of the Orphan Drug Act in making that progress possible.”
“It is critical to note that orphan drugs remain a sliver of overall drug spending in the U.S.,” Saltonstall said. “NORD remains committed to shining a light on the simple truths that illustrate how the Orphan Drug Act continues to be vital to the future of rare disease drug research and development.”
About 7,000 rare diseases have been identified, affecting approximately 30 million Americans. Many affect only a few hundred or a few thousand individuals. Rare diseases tend to be chronic, serious and life-threatening. More than 80 percent are believed to be genetic.
Information on the report, including a link to the study, is available on the NORD website at www.rarediseases.org/rareinsights.
Tuesday, October 16, 2018
IGF-1 Clinical Trial for Kennedy's Disease
The Lancet – Neurology published the following article yesterday on the IGF-1 clinical trial for Kennedy’s Disease (SBMA). Below are excerpts of the Summary. The full Summary can be read at the link below and the article can also be purchased on the website.
Safety, tolerability, and preliminary efficacy of an IGF-1 mimetic in patients with spinal and bulbar muscular atrophy: a randomised, placebo-controlled trial
Summary
Background
“Spinal and bulbar muscular atrophy is an X-linked neuromuscular disease caused by CAG repeat expansion in the androgen receptor gene. Patients with this disease have low concentrations of insulin-like growth factor-1 (IGF-1), and studies of overexpression and administration of IGF-1 showed benefit in a transgenic model; thus the IGF-1 pathway presents as a potential treatment target. We assessed safety, tolerability, and preliminary efficacy of BVS857, an IGF-1 mimetic, in patients with spinal and bulbar muscular atrophy. …”
Methods
“In this randomised, double-blind, placebo-controlled trial, we recruited patients from neuromuscular centres in Denmark (Copenhagen), Germany (Ulm), Italy (Padova), and three sites within the USA (Bethesda, MD; Irvine, CA; and Columbus, OH). …”
Findings
“31 patients were assessed for eligibility, 27 of whom were randomly assigned to either BVS857 treatment (n=18) or placebo (n=9), and 24 were included in the preliminary efficacy analysis (BVS857 group, n=15; placebo group, n=9). BVS857 was generally safe with no serious adverse events. No significant differences were found in adverse events between the BVS857 and placebo groups. …”
Interpretation
“TMV (thigh muscle volume) remained stable in patients with spinal and bulbar muscular atrophy after being given BVS857 for 12 weeks. The intervention was associated with high incidence of immunogenicity and did not improve muscle strength or function. Additional studies might be needed to assess the efficacy of activating the IGF-1 pathway in this disease. …”
Note: There is an accompanying article also noted:
Image: http://www.hgh-pro.com/igf-1.html
Saturday, October 13, 2018
Biomarkers of Spinal and Bulbar Muscle Atrophy
This report was published in Frontiers of Neurology three days ago. Excerpts are below and the entire report ban be read by following the link.
A biomarker is a parameter that can be measured accurately and reproducibly and used as an indicator of normal biological processes, pathogenic processes, or pharmacologic responses to a therapeutic intervention (WHO definition, 1998). An ideal biomarker should have a predictive value and capture subtle changes over relatively short periods of time. Additional requirements to biomarkers include cost-effectiveness, non-invasiveness, and reproducibility. It is generally agreed that no single biomarker is suitable for diagnostic, prognostic and monitoring roles and a panel of several markers may be better suited as multirole indicators. SBMA is a rare and slowly progressing condition, therefore the development of sensitive outcome measures would enable smaller sample-size and shorter duration of pharmaceutical trials.
In recent years, an unprecedented interest has developed in the standardized assessment of neuromuscular performance in SBMA, evaluation of novel therapeutic strategies and in the launch of national SBMA registries. Many of the commonly used instruments, such as the MRC score, respiratory function parameters, the modified Norris scale, ALSFRS-r, Quantitative Myasthenia Gravis Score etc. are non-specific to SBMA, yet remain widely utilized. As these tools have been developed for other conditions, new batteries of tests have been recently proposed to specifically appraise disability in SBMA.
Interest in SBMA biomarkers has grown steadily in recent years, fuelled both by accruing knowledge about pathogenesis and novel therapeutic strategies. SBMA is now widely recognized as a multisystem syndrome. A multitude of studies focus on multi-organ involvement, and the systemic phenotype is now considered just as relevant as the neurological manifestations. It is increasingly recognized that non-neurological features of the disease have an equally important impact on the patients' quality of life. Until now, clinical trials on SBMA focused almost exclusively on the treatment of motor symptoms, but a shift to targeted molecular therapies and focus on systemic processes are likely to be witnessed in the near future. From a clinical trial perspective, ideal biomarkers should undergo robust validation, sensitivity and specificity profiling, and sampling and measurement harmonization across different centers. Crucially, candidate markers should be able to detect the subtle changes expected after the administration of a specific treatment. Given the particularly slow progression rates observed in SBMA, the definition of an effective outcome measures is challenging. The integration of neurological, metabolic, and endocrine indicators seems essential into composite biomarker panels in addition to functional scales. Serum creatinine levels appear to correlate strongly with motor impairment and HOMA-IR index with disease duration. The convincing validation of these parameters and their use as effective outcome measures in clinical trials will require robust multicenter study designs.
Biomarkers of Spinal and Bulbar Muscle Atrophy (SBMA): A Comprehensive Review
Biomarkers in SBMA
A biomarker is a parameter that can be measured accurately and reproducibly and used as an indicator of normal biological processes, pathogenic processes, or pharmacologic responses to a therapeutic intervention (WHO definition, 1998). An ideal biomarker should have a predictive value and capture subtle changes over relatively short periods of time. Additional requirements to biomarkers include cost-effectiveness, non-invasiveness, and reproducibility. It is generally agreed that no single biomarker is suitable for diagnostic, prognostic and monitoring roles and a panel of several markers may be better suited as multirole indicators. SBMA is a rare and slowly progressing condition, therefore the development of sensitive outcome measures would enable smaller sample-size and shorter duration of pharmaceutical trials.
Biomarkers of Neurological Involvement in SBMA
In recent years, an unprecedented interest has developed in the standardized assessment of neuromuscular performance in SBMA, evaluation of novel therapeutic strategies and in the launch of national SBMA registries. Many of the commonly used instruments, such as the MRC score, respiratory function parameters, the modified Norris scale, ALSFRS-r, Quantitative Myasthenia Gravis Score etc. are non-specific to SBMA, yet remain widely utilized. As these tools have been developed for other conditions, new batteries of tests have been recently proposed to specifically appraise disability in SBMA.
Discussion and Future Perspectives
Interest in SBMA biomarkers has grown steadily in recent years, fuelled both by accruing knowledge about pathogenesis and novel therapeutic strategies. SBMA is now widely recognized as a multisystem syndrome. A multitude of studies focus on multi-organ involvement, and the systemic phenotype is now considered just as relevant as the neurological manifestations. It is increasingly recognized that non-neurological features of the disease have an equally important impact on the patients' quality of life. Until now, clinical trials on SBMA focused almost exclusively on the treatment of motor symptoms, but a shift to targeted molecular therapies and focus on systemic processes are likely to be witnessed in the near future. From a clinical trial perspective, ideal biomarkers should undergo robust validation, sensitivity and specificity profiling, and sampling and measurement harmonization across different centers. Crucially, candidate markers should be able to detect the subtle changes expected after the administration of a specific treatment. Given the particularly slow progression rates observed in SBMA, the definition of an effective outcome measures is challenging. The integration of neurological, metabolic, and endocrine indicators seems essential into composite biomarker panels in addition to functional scales. Serum creatinine levels appear to correlate strongly with motor impairment and HOMA-IR index with disease duration. The convincing validation of these parameters and their use as effective outcome measures in clinical trials will require robust multicenter study designs.
Wednesday, October 10, 2018
Beyond motor neurons
This is a pretty good recap of what we know and what else might be of importance in finding a treatment or cure for Kennedy's Disease.
The entire post can be found here:
Extra-motor neuron features in SBMA, such as primary muscle atrophy or hormonal abnormalities, are emerging as clinically highly impactful in patients’ quality of life and disease progression. Their thorough investigations are proving critical for a number of reasons. First, they may provide important insights into common mechanisms of pathogenesis. Second, the peripheral abnormalities may offer the opportunity for direct functional assessments and repetitive samplings, therefore representing potentially exploitable biomarkers to track disease progression and/or response to therapy. Lastly, disentangling the underlying molecular mechanisms of this highly integrated inter-tissues cross-talk may offer unparalleled opportunities for therapeutic interventions in the near future.
The entire post can be found here:
Beyond motor neurons: expanding the clinical spectrum in Kennedy’s disease
The conclusions are shown below:Conclusions
In SBMA, as in other genetic conditions caused by mutations in ubiquitously expressed genes, the clinical picture is the result of a complex interplay between differentially affected tissues, which struggle to cooperate to maintain homeostasis.Extra-motor neuron features in SBMA, such as primary muscle atrophy or hormonal abnormalities, are emerging as clinically highly impactful in patients’ quality of life and disease progression. Their thorough investigations are proving critical for a number of reasons. First, they may provide important insights into common mechanisms of pathogenesis. Second, the peripheral abnormalities may offer the opportunity for direct functional assessments and repetitive samplings, therefore representing potentially exploitable biomarkers to track disease progression and/or response to therapy. Lastly, disentangling the underlying molecular mechanisms of this highly integrated inter-tissues cross-talk may offer unparalleled opportunities for therapeutic interventions in the near future.
Monday, October 8, 2018
Planning for Long-Term Care: The Costs and Potential Issues
A special "thank you" to Hazel Bridges who has written another informative article on long-term care.
Long-Term Care
Planning
for long-term care can be tricky, to
say the least; you never know what might happen in the next five or 10 years,
and it can be difficult to think about financial planning when you’re unsure of
what the future may bring. For seniors, however, it’s imperative to start
thinking about how you might pay for your care should you need to stay in a
hospital or nursing facility for an extended amount of time. Health insurance
and Medicare are wonderful resources, but they only cover so much of the cost associated with
long-term care.
For
now, think about how to boost your savings and ensure that you are doing
everything in your power to prevent issues down the road. This means making
your health and mobility a priority and making changes to your home to make
it more accessible. This will ensure that you are able to live in it longer,
even if your health should fall into decline, and that you will stay safe.
Keep
reading for some great tips on how to plan for long-term care.
Turn Your Home Into a Safe Haven
Prevention
is one of the best ways to ensure that your health and safety are a priority.
Making changes to your home is a great way to start, as it will help you remain
there longer without the need for an assisted living facility. For example, you
might add grab bars in the shower, place sturdy railings on both sides of the
stairs, widen doorways to allow for medical equipment, add lighting to prevent
falls, or remove loose rugs or carpeting that can be trip hazards. Think about
what each room in your home needs in regard to safety and comfort, and do a
little research to figure out what the cost will be to make the changes. Check
out this guide for some great tips on
which changes you should make and how to get started.
Know Your Policies
You
may have a health insurance policy that will help pay for care down the road,
but how much will it cover in the long term? Take a good look at your policy,
and carefully read over your Medicare or Medicaid paperwork to see exactly
what you will be responsible for should you need long-term or daily care due to
an injury or major health issue.
Consider Selling Your Life Insurance Policy
If
you need a large sum of money to cover care costs, or if you just want to pad
your savings account, consider selling your life insurance policy or see if
your policy offers a cash value option that would allow
you to take money from the total benefit amount now. This will reduce the
amount that your loved ones would receive in the event of your death, but it
could be a viable option if you need cash to pay medical bills or to put aside
for your future needs.
Make Lifestyle Changes
Along
with the changes to your home, you can make changes to your lifestyle that will allow you to
stay healthy, which, in turn, can possibly reduce the risk that you will need
long-term care down the road. This includes eating right, getting daily
exercise, and eliminating bad habits, such as smoking or using substances such
as alcohol to excess.
Planning
for long-term care does not have to be stressful. By starting now, you are on
the right track toward ensuring that your healthcare needs won’t be
overwhelming in the future. Make the necessary changes to help your body and mind
stay healthy, and remember to ask for help when you need it.
Photo
via Pixabay by Sabinevanerp
Monday, October 1, 2018
Symptoms of Kennedy's Disease (SBMA)
Any time I list the potential symptoms of Kennedy’s Disease, aka Spinal Bulbar Muscular Atrophy (SBMA), there is a tendency for someone to comment, “I have that. Do you think it’s Kennedy’s Disease?”
My answer is always the same. “I don’t know. You need to see your primary care doctor and discuss your symptoms with her/him.”
When my symptoms started, there was no DNA test for Kennedy’s Disease (SBMA). Most doctors and many neurologists did not know about SBMA. Neurologists put you through a series of tests, some not very pleasant, to help determine the cause of the symptoms. Most often, it was an educated guess based upon available evidence. In my case, I was diagnosed with ALS.
Several years later, another doctor diagnosed it as SBMA and sent me to see Dr. Fischbeck for a second opinion. I still remember walking into Dr. Fischbeck’s office that morning. He saw my gate, nodded his head, and said, “You have the walk.” He performed a DNA test and confirmed Kennedy’s Disease.
Today, because of the DNA test, a doctor can draw a little blood and send it off to a lab. Within a few weeks you will have an answer as to if you have Kennedy’s Disease. If not, you will still have to go through more testing, but at least SBMA is ruled out.
In regards to the list of symptoms below, those of us living with Kennedy’s Disease normally do not have all of them. We will have several and some might not appear until later in the progression. The most common early symptoms are severe cramping, hand tremors, unexplained fasciculations, and gynecomastia.
Please note there is a wealth of information available on the Kennedy’s Disease Association website (http://www.kennedysdisease.org/index.php/about-kennedys-disease/what-is-kennedys-disease).
My answer is always the same. “I don’t know. You need to see your primary care doctor and discuss your symptoms with her/him.”
When my symptoms started, there was no DNA test for Kennedy’s Disease (SBMA). Most doctors and many neurologists did not know about SBMA. Neurologists put you through a series of tests, some not very pleasant, to help determine the cause of the symptoms. Most often, it was an educated guess based upon available evidence. In my case, I was diagnosed with ALS.
Several years later, another doctor diagnosed it as SBMA and sent me to see Dr. Fischbeck for a second opinion. I still remember walking into Dr. Fischbeck’s office that morning. He saw my gate, nodded his head, and said, “You have the walk.” He performed a DNA test and confirmed Kennedy’s Disease.
Today, because of the DNA test, a doctor can draw a little blood and send it off to a lab. Within a few weeks you will have an answer as to if you have Kennedy’s Disease. If not, you will still have to go through more testing, but at least SBMA is ruled out.
In regards to the list of symptoms below, those of us living with Kennedy’s Disease normally do not have all of them. We will have several and some might not appear until later in the progression. The most common early symptoms are severe cramping, hand tremors, unexplained fasciculations, and gynecomastia.
Please note there is a wealth of information available on the Kennedy’s Disease Association website (http://www.kennedysdisease.org/index.php/about-kennedys-disease/what-is-kennedys-disease).
SYMPTOMS(I apologize for the formatting problem below) |
Neurological:
|
|
Bulbar Signs
|
The Bulbar muscles are those supplied by the
motor nerves coming off the brain stem. They control breathing, swallowing,
talking and other functions of the throat. Bulbar signs are problems with
these functions.
|
Dysphagia
|
Trouble swallowing. (One of the Bulbar
signs.)
|
Intention Tremor
|
Hand tremors when trying to do something.
|
Normal Babinski
|
Normal plantar response, ie., when the bottom
of the foot is scraped, the toes bend down. An abnormal response would be an
upward bending of the toes indicating a problem in the brain itself.
|
Lower Motor Neuropathy
|
The lower motor nerves are those that run
from the spinal cord to the muscles that they stimulate to move. Loss of that
nerve leads to weakness and wasting of the muscle.
|
Primary Sensory Neuropathy
|
Numbness over certain areas. Loss of
sensation.
|
Decreased or Absent Deep Tendon Reflexes
|
When a doctor taps the knee with his
hammer there is no response.
|
Muscular:
|
|
Fasciculations
|
Twitching of small muscles without purposeful
movement. These can be seen through the skin.
|
Cramps
|
Large muscle spasms.
|
Postural Tremor
|
Shaky muscles with certain positions.
|
Muscular Atrophy
|
Wasting and shrinkage of muscles that occurs
when the lower motor nerve does not stimulate the muscle adequately.
|
Hypertrophied Calves
|
Calf muscles that become thicker because of
cramps.
|
Thoracic:
|
|
Gynecomastia
|
Enlarged breasts.
|
Endrocrine
|
|
Androgen Deficiency
|
Loss of masculinizing effect (qualities that
are perceived as masculine).
|
Estrogen Excess
|
More of an apparent estrogen effect because
of the lost of masulinizing effect.
|
Genito-Urinary:
|
|
Impotence
|
Erectile dysfunction.
|
Reduced Fertility
|
Low sperm count.
|
Testicular Atrophy
|
Testicles become smaller and less functional.
|
Miscellaneous Characteristics:
|
|
Late Apparent Onset
|
Symptoms could become apparent in 20's or
30's, but might not appear until the 60's or 70's.
|
Slow Progression
|
Near-normal lifespan.
|
Asymmetry of Clinical Signs
|
Muscles of one side may be more affected than
the same muscles on the other side.
|
Laboratory:
|
|
Elevated Serum Creatine Kinase
|
Elevation of CPK enzyme in the blood
test. Can be confused with the enzyme released during a heart attack.
|
Subscribe to:
Posts (Atom)