 As soon as I saw the New York Times’ article by Henry Fountain, “Human Muscle, Regrown on Animal Scaffolding,” I had to read it. The two page article was focused on how this new technology appears to be working for some soldiers returning from the war that need rehabilitation. However, the more I read the more I wondered if this might be something available for those of us living with Kennedy’s Disease.
As soon as I saw the New York Times’ article by Henry Fountain, “Human Muscle, Regrown on Animal Scaffolding,” I had to read it. The two page article was focused on how this new technology appears to be working for some soldiers returning from the war that need rehabilitation. However, the more I read the more I wondered if this might be something available for those of us living with Kennedy’s Disease.Excerpts from the article follow, but you can follow the above link to read the entire article.
___________________________
PITTSBURGH — In the months after a roadside bomb in Afghanistan blew off part of his left thigh, Sgt. Ron Strang wondered if he would ever be able to walk normally again.
The explosion and subsequent rounds of surgery left Sergeant Strang, 28, a Marine, with a huge divot in his upper thigh where the quadriceps muscle had been. He could move the leg backward, but with so much of the muscle gone he could not kick it forward. He could walk, but only awkwardly.
“I got really good at falling,” he said of his efforts. And Sergeant Strang, a tall, athletic man, had to give up running.
But that was two years ago. Now he walks easily, can run on a treadmill and is thinking of a post-military career as a police officer. “If you know me, or know to look for it, you can see a slight limp,” he said. “But everybody else, they go, ‘I would never have guessed.’ ”
There is something else they would never have guessed: Sergeant Strang has grown new muscle thanks to a thin sheet of material from a pig.
The material, called extracellular matrix, is the natural scaffolding that underlies all tissues and organs, in people as well as animals. It is produced by cells, and for years scientists thought that its main role was to hold them in their proper position.
But researchers now know that this scaffolding also signals the body to grow and repair those tissues and organs. Armed with that knowledge, the new body builders are using this material from pigs and other animals to engineer the growth of replacement tissue in humans.
The technique used on Sergeant Strang, though still in development, holds particular promise for some of the thousands of veterans of the Iraq and Afghanistan wars who have been maimed by explosives and have lost so much muscle from an arm or a leg that amputation is sometimes the best alternative.
_________________________________
Later the article further explained the process and got into more specifics.
_________________________________
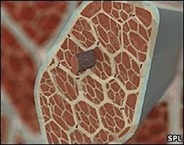 The scaffolding is isolated by stripping out all of the living cells from a tissue or organ, leaving an intricate three-dimensional web of proteins and other compounds. Removing the cells eliminates the possibility that the material, of animal origin, will be rejected outright by the body when it is implanted. But the matrix does provoke a less intense immune response, Dr. Badylak said, which is necessary for it to work. “You actually need the immune system to recognize the material.”
The scaffolding is isolated by stripping out all of the living cells from a tissue or organ, leaving an intricate three-dimensional web of proteins and other compounds. Removing the cells eliminates the possibility that the material, of animal origin, will be rejected outright by the body when it is implanted. But the matrix does provoke a less intense immune response, Dr. Badylak said, which is necessary for it to work. “You actually need the immune system to recognize the material.” “The body can say, ‘This is not me,’ but the signals that are there are actually telling me that I need to rebuild that tissue,” he added.
The matrix has to be in contact with healthy tissue, which is why scar tissue must be removed first. “If it’s put in the middle of a scar, it doesn’t remodel because it’s not exposed to the bloodstream and sources of cells,” Dr. Badylak said.
Stitching it directly to the muscle also ensures that it will be stretched when the muscle is activated, beginning the day after surgery, when patients start an intensive program of physical therapy. Putting a mechanical load on the matrix tells the body, in effect, that this should become muscle and not some other kind of tissue.
Sergeant Strang was skeptical when he first signed up for the trial and cleared all the physical hurdles to qualify for it — among other things, patients must have some muscle remaining and enough undamaged nerves so the muscle can work. But at that point he was willing to try anything to be able to walk normally again.
_________________________________
Well, after reading the article, I had to contact our resident biology professor and ask if this process might be applicable for someone with Kennedy’s Disease. Ed’s response was:
“It could, it would appear to depend on if there were any neurons left. The common belief is the muscles atrophy is due to the neurons dying. If there were no motor neurons, then it would seem that the muscle would not grow (note the need for the presence of muscle and nerves in the patient to be eligible for the procedure).”
Well, that wasn’t a definite “NO” anyway.

No comments:
Post a Comment
Please feel free to comment. By taking a moment to share your thoughts you add much to these articles. The articles then become more than just something I said or believe. In addition, by adding a comment, you might just be helping the next reader by sharing your opinion, experience, or a helpful tip. You can comment below or by sending me an email. I look forward to hearing from you.